|
Past paper questions
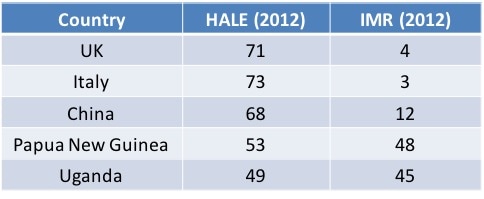
May 2013: Explain why health-adjusted life expectancy (HALE) is a better way to quantify the health of a community than infant mortality. (6 marks) May 2013 Mark Scheme: Infant mortality reflects health of mothers, nutrition, health care education and services. Many countries have reduced infant mortality with relatively small investments in health care services. Infant mortality is a “snap-shot”, reflecting a limited time period. The HALE includes many more health-related issues, and all age-groups. It also reflects a longer time period, including infant mortality, but also including mortality of other age-groups, and more importantly, ill-health throughout the population. Award up to [3 marks] for the explanation of how each measure is used to quantify health. For full marks, HALE must be clearly shown to be the better measure. |
How do we measure health variations?
Life expectancy: The average number of calories consumed by a person within a specific population per day.
Infant mortality rate: The average number of years that a person can expect to live in "full health", excluding the years lived in less than full health due to disease and/or injury.
Child mortality rate: The number of deaths of children less than one year of age per 1000 live births.
Health-adjusted life expectancy (HALE): The proportion of the population with access to an adequate amount of safe drinking water located within a convenient distance from the user’s dwelling.
Calorie intake: The average period that a person may expect to live.
Access to safe water: The number of doctors per 1000 (or 10,000) population.
Physician density (access to health services): The probability (expressed as a rate per 1000 live births) of a child born in a specified year dying before the age of 5.
Life expectancy: The average number of calories consumed by a person within a specific population per day.
Infant mortality rate: The average number of years that a person can expect to live in "full health", excluding the years lived in less than full health due to disease and/or injury.
Child mortality rate: The number of deaths of children less than one year of age per 1000 live births.
Health-adjusted life expectancy (HALE): The proportion of the population with access to an adequate amount of safe drinking water located within a convenient distance from the user’s dwelling.
Calorie intake: The average period that a person may expect to live.
Access to safe water: The number of doctors per 1000 (or 10,000) population.
Physician density (access to health services): The probability (expressed as a rate per 1000 live births) of a child born in a specified year dying before the age of 5.
1. How do we measure health?
Infant Mortality Rate: The number of babies who die before the age of 1. This statistic just demonstrates one aspect of a countries development. It does not take into consideration differences in healthcare systems, or the social status of women. It also doesn't consider the likelihood of a woman having a baby in hospital or the delivery methods of babies and the monitoring. This means that the statistic can become difficult when used as an indicator for how well a country is doing when it comes to measuring health.
HALE: Average number of years that a person can expect to live in "full health" by taking into account years lived in less than full health due to disease and/or injury.
Health-adjusted life expectancy (HALE) is a measurement developed by the World Health Organization that attempts to capture a more complete estimate of health than standard life expectancy rates (note that HALE was previously referred to as Disability-Adjusted Life Expectancy or DALE). HALE estimates the number of healthy years an individual is expected to live at birth by subtracting the years of ill health – weighted according to severity – from overall life expectancy. HALE is also calculated at age 65 to provide a measurement of the quality of life of seniors. By moving beyond mortality data, HALE is meant to measure not just how long people live, but the quality of their health through their lives
HALE: Average number of years that a person can expect to live in "full health" by taking into account years lived in less than full health due to disease and/or injury.
Health-adjusted life expectancy (HALE) is a measurement developed by the World Health Organization that attempts to capture a more complete estimate of health than standard life expectancy rates (note that HALE was previously referred to as Disability-Adjusted Life Expectancy or DALE). HALE estimates the number of healthy years an individual is expected to live at birth by subtracting the years of ill health – weighted according to severity – from overall life expectancy. HALE is also calculated at age 65 to provide a measurement of the quality of life of seniors. By moving beyond mortality data, HALE is meant to measure not just how long people live, but the quality of their health through their lives
2. Different health care systems.
Emergent
Pluralistic –
Insurance/social security –
National Health Service –
Socialised –
- Health care as an item of personal consumption.
- Healthcare viewed as an item of personal consumption.
- Physicians operate as solo entrepreneurs
- Professional associations are powerful
- Private ownership of facilities
- Direct payment to physicians
- State’s role in healthcare is minimal
- Development of local health workers
- Examples: Bangladesh, Brazil, India, Kenya, Pakistan, Sierra Leone, South Africa
Pluralistic –
- Health care as a consumer product.Health care viewed as a consumer product
- Physicians operate as solo entrepreneurs
- Professional associations are powerful
- Private and public ownership of facilities
- State’s role in healthcare is minimal and indirect
- Examples: USA
Insurance/social security –
- Health care as an insured/guaranteed consumer product.
- Physicians operate as solo entrepreneurs and as members of professional associations, which are strong
- Private and public ownership of facilities
- Payment for services mostly indirect
- State’s role in healthcare is evident but indirect
- Examples: France, Japan, Spain
National Health Service –
- Healthcare is a state-supported service
- Physicians operate as solo entrepreneurs and as members of professional associations, which are strong
- Facilities are mainly publicly owned
- State’s role in healthcare is central and direct
- Health care as a state supported service
- Examples: Canada, UK
Socialised –
- Health care as a state-provided public service
- Physicians are state-employed
- Professional associations are weak or non-existent
- Facilities are wholly publicly owned
- Payments for services are entirely indirect (tax)
- State’s role in healthcare is total
- Examples: China, Cuba
3. Comparing health care
Cuba- a socialised system
Key statistics (Cuba):
- Very effective: the WHO ranks it at a level just below that of the USA, despite spending ten times less per person.
- Operated by the Cuban government which assumes fiscal and administrative responsibility for the health care of all its citizens. No private hospitals or clinics are permitted.
- 30,000 family doctors and 10,000 dentists serve a population of 11 million.
- 21 medical schools provide free training.
The main principle is outlined in Article 50 of the revised Cuban Constitution (1976):
Everyone has the right to health protection and care. The state guarantees this right by providing free medical and hospital care by means of the installations of the rural medical service network, polyclinics, hospitals, preventative and specialized treatment centers; by providing free dental care; by promoting the health publicity campaigns, health education, regular medical examinations, general vaccinations and other measures to prevent the outbreak of disease.
Cuban healthcare and the Global Community:
- Cuba has been able to export primary care practitioners and specialists for periods of service in other Third World nations, as the education of physicians came to exceed the country's internal requirements.
- Since the Chernobyl nuclear plant exploded in 1986, more than 20,000 children from Ukraine, Belarus and Russia have traveled to Cuba for treatment of radiation sickness and psychologically based problems associated with the radiation disaster.
- Cuba attracts nearly 20,000 paying health tourists, generating revenues of around $40m a year for the Cuban economy.
How does Cuban healthcare compare?
Despite withdrawal of Soviet funding and the trade embargoes imposed by the US…
- The chance of a Cuban child dying at five years of age or younger is 7 per 1000 live births in Cuba, while it's 8 per 1000 in the US.
- Cuba has nearly twice as many physicians as the U.S. – 6.72 doctors per thousand people compared to 2.42 doctors per thousand, according to WHO.
Criticisms and Problems:
- Low pay of doctors (only $15 per month). This has led to many doctors defecting to other countries to access higher wages.
- Poor facilities (buildings have been described as in a poor state of repair and mostly outdated).
- Poor provision of equipment (some surgeons have complained that they have had to re-use latex gloves, for example).
- Frequent absence of essential drugs (e.g. aspirin and basic antibiotics) has led to the use of a ‘black market’ health system (‘sociolismo’).
- Complaints that foreign "health tourists" paying with dollars, and senior Communist party officials, receive a higher quality of care than Cuban citizens.
USA- a pluralistic system
Key statistics (USA):
What is America’s healthcare like?
- There is no nationwide system of government-owned medical facilities that is open to the general public.
- Instead, the health system is provided by thousands of independent doctors, pharmacies, clinics and hospitals. The consumer pays for out-patient treatment, doctors’ fees, hospitalisation, surgery, equipment and appliances. Most people have insurance cover to pay for treatment, although it is estimated that there are 44 million inhabitants without insurance.
- There is some healthcare provided by the Federal Government for vulnerable populations such as the elderly and the poor, but this is only basic.
How does American healthcare compare?
- The United States is the "only wealthy, industrialized nation that does not ensure that all citizens have coverage" (i.e. some kind of insurance) according to the Institute of Medicine.
- A recent study found that between 1997 and 2003, preventable deaths declined more slowly in the United States than in 18 other industrialized nations.
Equality and Access
- Around 84.7% of citizens have some form of health insurance; either through their employer or the employer of their spouse or parent (59.3%), purchased individually (8.9%), or provided by government programs.
- Recent studies find growing gaps in life expectancy based on income and geography.
- All government health care programmes have restricted eligibility, and there is no national system of health insurance which guarantees that all citizens have access to health care.
- Individuals with private or government insurance must generally find a medical facility which accepts the particular type of medical insurance they carry.
- However, The Emergency Medical Treatment and Active Labor Act requires virtually all hospitals to accept all patients, regardless of the ability to pay, for emergency room care.
Criticisms and Problems:
- Health insurance costs are rising faster than wages or inflation, and medical causes were cited by approximately half of bankruptcy filers in the USA in 2001.
- Some Americans do not qualify for government-provided health insurance, are not provided health insurance by an employer, and are unable to afford, or choose not to purchase, private health insurance. When charity or "uncompensated" care is not available, they sometimes simply go without needed medical treatment.
- Ethnic minorities such as African Americans, Native Americans, Asian Americans, and Hispanics have a higher incidence of chronic diseases, higher mortality, and poorer health outcomes compared to ‘Whites’ (as access to healthcare is undoubtedly linked to socio-economic background).
- During the 1990s, the price of prescription drugs became a major issue in American politics as the prices of many new drugs increased exponentially, and many citizens discovered that neither the government nor their insurer would cover the cost of such drugs.
The UK- the National Health Service
Key statistics (UK):
What is the NHS?
- Founded in 1948
- The essence of a satisfactory health service is that rich and poor are treated alike.
- Now operates primarily through ‘Primary Care Trusts’ (PCTs)
- Provides free healthcare to all permanent UK residents
- Paid for through general taxation
- Private healthcare is, however, available
How It Operates:
Its core principles include:
- providing a universal service for all based on clinical need, not ability to pay
- responding to the different needs of different populations
- using public funds for healthcare solely for NHS patients
Funding and Organisation
- Funded from general taxation, including contributions from National Insurance payments.
- 2008/9 total budget for Dept of Health = £94bn, of which £92.5bn went to the NHS.
- The NHS is the world’s largest health service, and the world’s fourth-largest employer.
- Controlled by the UK government through the Dept of Health
- Organised into a series of regional PCTs, as well as national services including NHS Direct.
Criticisms and Problems:
- The NHS does not offer all potential treatments for illnesses and disease if deemed cost ineffective e.g. homeopathy.
- Increased demand for healthcare leads to continual pressure on political bodies to increase spending and widen the range of treatments available.
- Taxpayers who choose to pay for private healthcare must nonetheless still contribute to the NHS via taxation.
- Waiting lists vary widely between regions of the UK. Plus, the lack of availability of some treatments due to their perceived poor cost-effectiveness sometimes leads to what some call a "postcode lottery".
- Criticisms regarding the standard of hygiene across the NHS e.g. outbreaks of ‘superbugs’ such as MRSA. The introduction of Private Finance Initiative cleaning contractors into the NHS and the associated "cutting corners on cleaning" have been blamed for the problem.
- Some hospitals and trusts across the UK are now running financial deficits and getting into debt.
- ‘Bed blockers’ e.g. geriatric patients awaiting a place in a nursing or residential facility – can prevent others receiving treatment.
Key statistics (Cuba):
- Life expectancy at birth m/f (years): 76/80
- Total expenditure on health as % of GDP (2012): 10.6
- Private expenditure on health as % total expenditure on health (2005): 9.2
- Very effective: the WHO ranks it at a level just below that of the USA, despite spending ten times less per person.
- Operated by the Cuban government which assumes fiscal and administrative responsibility for the health care of all its citizens. No private hospitals or clinics are permitted.
- 30,000 family doctors and 10,000 dentists serve a population of 11 million.
- 21 medical schools provide free training.
The main principle is outlined in Article 50 of the revised Cuban Constitution (1976):
Everyone has the right to health protection and care. The state guarantees this right by providing free medical and hospital care by means of the installations of the rural medical service network, polyclinics, hospitals, preventative and specialized treatment centers; by providing free dental care; by promoting the health publicity campaigns, health education, regular medical examinations, general vaccinations and other measures to prevent the outbreak of disease.
Cuban healthcare and the Global Community:
- Cuba has been able to export primary care practitioners and specialists for periods of service in other Third World nations, as the education of physicians came to exceed the country's internal requirements.
- Since the Chernobyl nuclear plant exploded in 1986, more than 20,000 children from Ukraine, Belarus and Russia have traveled to Cuba for treatment of radiation sickness and psychologically based problems associated with the radiation disaster.
- Cuba attracts nearly 20,000 paying health tourists, generating revenues of around $40m a year for the Cuban economy.
How does Cuban healthcare compare?
Despite withdrawal of Soviet funding and the trade embargoes imposed by the US…
- The chance of a Cuban child dying at five years of age or younger is 7 per 1000 live births in Cuba, while it's 8 per 1000 in the US.
- Cuba has nearly twice as many physicians as the U.S. – 6.72 doctors per thousand people compared to 2.42 doctors per thousand, according to WHO.
Criticisms and Problems:
- Low pay of doctors (only $15 per month). This has led to many doctors defecting to other countries to access higher wages.
- Poor facilities (buildings have been described as in a poor state of repair and mostly outdated).
- Poor provision of equipment (some surgeons have complained that they have had to re-use latex gloves, for example).
- Frequent absence of essential drugs (e.g. aspirin and basic antibiotics) has led to the use of a ‘black market’ health system (‘sociolismo’).
- Complaints that foreign "health tourists" paying with dollars, and senior Communist party officials, receive a higher quality of care than Cuban citizens.
USA- a pluralistic system
Key statistics (USA):
- Life expectancy at birth m/f (years): 75/80
- Total expenditure on health as % of GDP (2012): 17.9
- Private expenditure on health as % total expenditure on health (2005): 54.9
What is America’s healthcare like?
- There is no nationwide system of government-owned medical facilities that is open to the general public.
- Instead, the health system is provided by thousands of independent doctors, pharmacies, clinics and hospitals. The consumer pays for out-patient treatment, doctors’ fees, hospitalisation, surgery, equipment and appliances. Most people have insurance cover to pay for treatment, although it is estimated that there are 44 million inhabitants without insurance.
- There is some healthcare provided by the Federal Government for vulnerable populations such as the elderly and the poor, but this is only basic.
How does American healthcare compare?
- The United States is the "only wealthy, industrialized nation that does not ensure that all citizens have coverage" (i.e. some kind of insurance) according to the Institute of Medicine.
- A recent study found that between 1997 and 2003, preventable deaths declined more slowly in the United States than in 18 other industrialized nations.
Equality and Access
- Around 84.7% of citizens have some form of health insurance; either through their employer or the employer of their spouse or parent (59.3%), purchased individually (8.9%), or provided by government programs.
- Recent studies find growing gaps in life expectancy based on income and geography.
- All government health care programmes have restricted eligibility, and there is no national system of health insurance which guarantees that all citizens have access to health care.
- Individuals with private or government insurance must generally find a medical facility which accepts the particular type of medical insurance they carry.
- However, The Emergency Medical Treatment and Active Labor Act requires virtually all hospitals to accept all patients, regardless of the ability to pay, for emergency room care.
Criticisms and Problems:
- Health insurance costs are rising faster than wages or inflation, and medical causes were cited by approximately half of bankruptcy filers in the USA in 2001.
- Some Americans do not qualify for government-provided health insurance, are not provided health insurance by an employer, and are unable to afford, or choose not to purchase, private health insurance. When charity or "uncompensated" care is not available, they sometimes simply go without needed medical treatment.
- Ethnic minorities such as African Americans, Native Americans, Asian Americans, and Hispanics have a higher incidence of chronic diseases, higher mortality, and poorer health outcomes compared to ‘Whites’ (as access to healthcare is undoubtedly linked to socio-economic background).
- During the 1990s, the price of prescription drugs became a major issue in American politics as the prices of many new drugs increased exponentially, and many citizens discovered that neither the government nor their insurer would cover the cost of such drugs.
The UK- the National Health Service
Key statistics (UK):
- Life expectancy at birth m/f (years): 77/81
- Total expenditure on health as % of GDP (2012): 9.6
- Private expenditure on health as % total expenditure on health (2005): 12.9
What is the NHS?
- Founded in 1948
- The essence of a satisfactory health service is that rich and poor are treated alike.
- Now operates primarily through ‘Primary Care Trusts’ (PCTs)
- Provides free healthcare to all permanent UK residents
- Paid for through general taxation
- Private healthcare is, however, available
How It Operates:
Its core principles include:
- providing a universal service for all based on clinical need, not ability to pay
- responding to the different needs of different populations
- using public funds for healthcare solely for NHS patients
Funding and Organisation
- Funded from general taxation, including contributions from National Insurance payments.
- 2008/9 total budget for Dept of Health = £94bn, of which £92.5bn went to the NHS.
- The NHS is the world’s largest health service, and the world’s fourth-largest employer.
- Controlled by the UK government through the Dept of Health
- Organised into a series of regional PCTs, as well as national services including NHS Direct.
Criticisms and Problems:
- The NHS does not offer all potential treatments for illnesses and disease if deemed cost ineffective e.g. homeopathy.
- Increased demand for healthcare leads to continual pressure on political bodies to increase spending and widen the range of treatments available.
- Taxpayers who choose to pay for private healthcare must nonetheless still contribute to the NHS via taxation.
- Waiting lists vary widely between regions of the UK. Plus, the lack of availability of some treatments due to their perceived poor cost-effectiveness sometimes leads to what some call a "postcode lottery".
- Criticisms regarding the standard of hygiene across the NHS e.g. outbreaks of ‘superbugs’ such as MRSA. The introduction of Private Finance Initiative cleaning contractors into the NHS and the associated "cutting corners on cleaning" have been blamed for the problem.
- Some hospitals and trusts across the UK are now running financial deficits and getting into debt.
- ‘Bed blockers’ e.g. geriatric patients awaiting a place in a nursing or residential facility – can prevent others receiving treatment.